As we all know, tuberculosis (TB) has been a topic of discussion in the global health community for centuries. It is a disease caused by the bacterium Mycobacterium tuberculosis, and despite being curable for many years, tuberculosis continues to affect millions of people each year. What we often forget is how susceptible children are to this disease, particularly those living in countries such as Sri Lanka. Today, we’ll look at the history of tuberculosis in Sri Lankan children, including its causes, risks, diagnosis, and how we can combat it together.
Understanding Tuberculosis as a Silent Threat
We know that tuberculosis does not affect just one part of the body. Although it primarily affects the lungs, a condition known as pulmonary tuberculosis, it can spread to other parts of the body, resulting in extrapulmonary TB. When tuberculosis (TB) spreads to the brain or spine, it can cause severe complications. Consider a child with tuberculosis meningitis, in which the bacteria have infected the brain lining. Severe headaches, confusion, and even seizures are among the possible symptoms. It’s frightening to consider, but this is the reality for some Sri Lankan children.
Types of Tuberculosis
As we proceed, we should remember that there are two major types of tuberculosis
01. Pulmonary Tuberculosis (PTB)
This is the most contagious form because it attacks the lungs and the bacteria spread through the air when an infected person coughs or sneezes. If a child inhales these bacteria, they too may become infected. This type of tuberculosis is more visible, but it can still go unnoticed if parents or caregivers fail to recognize symptoms such as a persistent cough or fever.
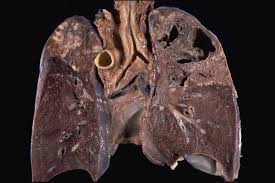
02. Extrapulmonary Tuberculosis (EPTB)
TB spreads beyond the lungs to lymph nodes, bones, and abdomen. It can even reach the brain, resulting in tuberculosis meningitis, one of the disease’s most dangerous forms. This type of tuberculosis is especially concerning for children because it can result in serious complications if not treated promptly.
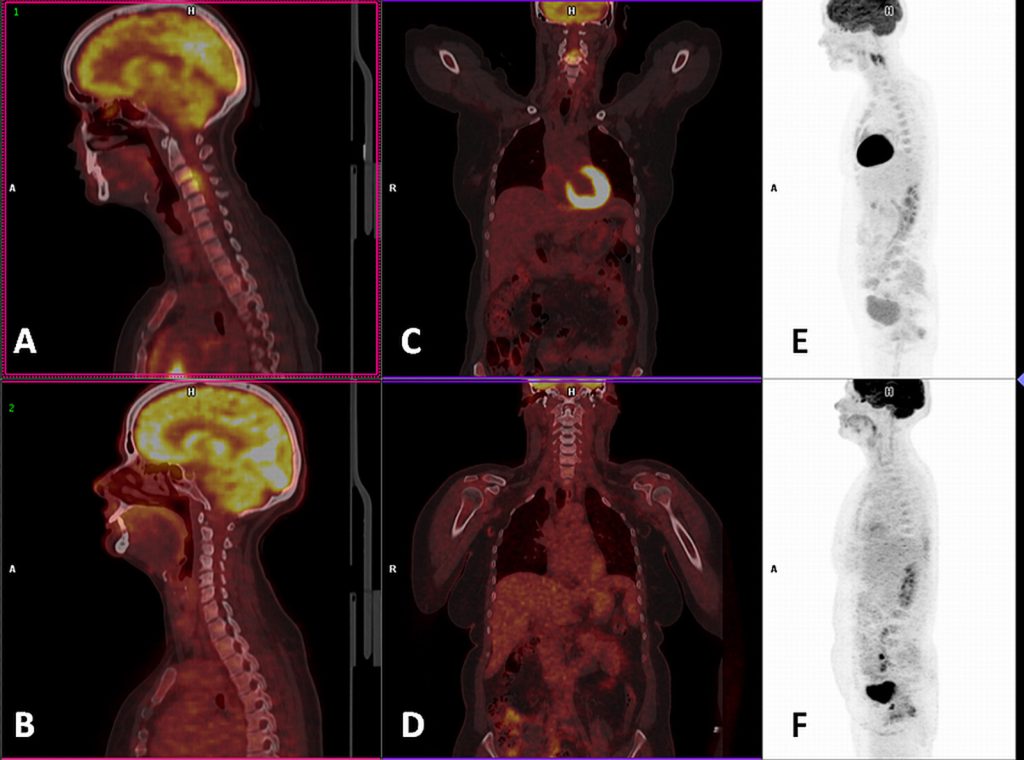
The Effects of Tuberculosis on Children in Sri Lanka
Let’s now examine the case of tuberculosis in children from Sri Lanka. Even though the overall figures may not seem like much—roughly 3% to 4% of all cases in Sri Lanka are in children—TB remains a serious public health issue. Approximately 140,000 children worldwide die from tuberculosis each year, out of an estimated one million who are afflicted.
Many youngsters in Sri Lanka get tuberculosis (TB) as a result of extended interaction with infected adults in their homes. Imagine that an adult, possibly a parent or grandparent, has tuberculosis (TB) but is unaware of it or has not finished their treatment. They frequently live in close quarters and unintentionally transfer the bacterium to their offspring over time. These kids are at risk of contracting severe types of tuberculosis if they are not diagnosed and treated early.
Risk Elements: Who Is Most at Risk?
It is important to keep in mind that certain youngsters are more vulnerable to tuberculosis than others. A child’s health and living circumstances are equally as important as whether or not they are exposed to tuberculosis.
Close contact with individuals infected with tuberculosis
Living with an adult who has tuberculosis is the most prevalent route for children to contract the disease. These adults are like ticking time bombs, spreading the bacterium to nearby youngsters, especially if they have untreated or inadequately treated pulmonary tuberculosis.
Immune system weakness
Children who already have illnesses that compromise their immune systems, such as HIV, are at a higher risk of contracting tuberculosis and experiencing its most severe symptoms. We know that children with HIV have more aggressive TB and are more likely to get TB meningitis.
Malnutrition and substandard living conditions
Poverty is a major issue in Sri Lanka, as it is in many other countries. Malnourished children lack the strength to fend against illnesses like tuberculosis. Furthermore, the ideal conditions for the spread of tuberculosis are crowded living quarters and inadequate ventilation, which are prevalent in low-income communities.
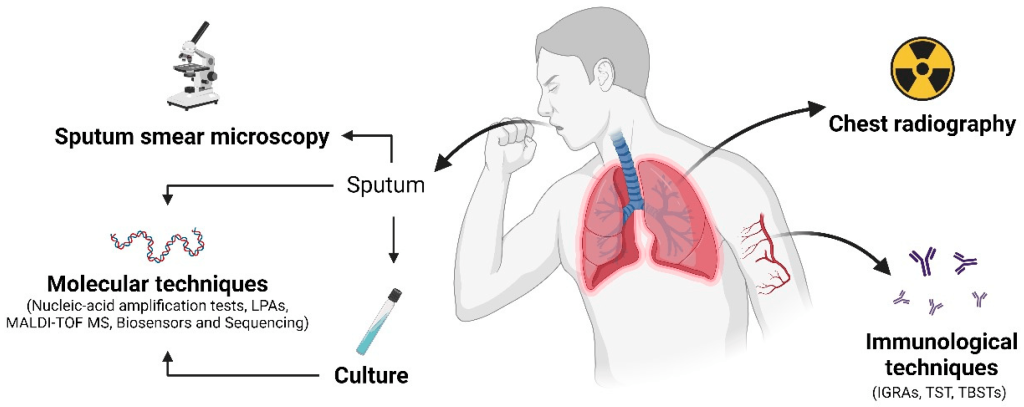
This figure illustrates relevant diagnostic techniques employed for pulmonary tuberculosis diagnosis. https://www.mdpi.com/2079-9721/12/9/202
How Can Tuberculosis in Children Be Diagnosed?
How can we determine whether a youngster has tuberculosis, then? Since children frequently don’t exhibit the same traditional symptoms as adults, diagnosing tuberculosis in them can be challenging. Young children’s symptoms may mimic those of other illnesses, and they may not be able to generate the sputum samples required for testing.
Clinical history and contact tracing
Doctors usually start by looking at the child’s history—have they been coughing for more than two weeks? Have they lost weight recently? Has anyone in their household had TB? These questions are crucial in determining whether further testing is needed.
Tuberculin Skin Test (TST)
This is one of the oldest tests for TB. A small amount of tuberculin is injected just under the skin, and after a couple of days, the area is checked for a reaction. If the skin swells up, it could mean the child has been exposed to TB. But the test doesn’t tell us if the infection is active or not.
Chest X-rays
For children, chest X-rays are often used to detect signs of TB in the lungs. If a child has pulmonary TB, the X-ray may show spots or cavities in the lungs that indicate infection.
New diagnostic tools
These days, Sri Lanka’s healthcare system is also using newer methods like the GeneXpert test. This test not only detects the TB bacteria but also tells doctors if the bacteria are resistant to rifampicin, one of the key TB drugs
The Long Road to Treating Tuberculosis in Children
What happens if a child is diagnosed with tuberculosis? Although treating tuberculosis is a drawn-out process, when done correctly, it works. Four medications are typically used to treat tuberculosis in children: isoniazid, rifampicin, pyrazinamide, and ethambutol. Though it can sometimes last longer, the course of treatment typically lasts six months. We are aware of how important it is to follow this treatment strategy. The TB germs may return stronger and more drug-resistant if a child does not complete the entire course. We refer to this as multidrug-resistant tuberculosis (MDR-TB). This results in a longer and more complex course of treatment that can continue up to 18 months or longer.
The problem is that families find it difficult to follow the treatment plan in many low-income communities. It might be burdensome due to the lengthy duration, possible adverse effects, and requirement for frequent hospital stays. Unfortunately, this leads to poor treatment adherence, which is a fundamental reason why drug-resistant TB is a developing problem.
Preventing Tuberculosis: Can We Stop It Before It Starts?
As we now know, prevention is just as important as treatment in the fight against tuberculosis. Every child in Sri Lanka is vaccinated against BCG soon after birth. Although it doesn’t totally prevent children from developing pulmonary TB, this vaccine helps protect against the more serious types of TB, such as TB meningitis.
Contact tracing is another important preventative measure. Doctors make sure to test everyone in the household, especially the youngsters, when an adult in the household is diagnosed with tuberculosis. Isoniazid preventative therapy (IPT) may be administered to a child who has been exposed to tuberculosis (TB) but is not yet exhibiting symptoms in order to prevent the germs from becoming active.
The Challenges Ahead
The Obstacles That Remain We are aware that despite all of the efforts, there are still a lot of challenges in the fight against tuberculosis in children. The largest problem is delayed diagnosis; far too frequently, TB is misdiagnosed as something else, and by the time it is discovered, the child’s illness has gotten worse. Poor treatment adherence is another problem we deal with. Multidrug-resistant TB spreads because the bacteria become more resistant if families don’t finish the therapy.
The Way Forward
The Path Ahead We must keep in mind that tuberculosis is a treatable illness as we finish this chapter in the history of the disease in Sri Lankan youngsters. We can lower the number of children who have tuberculosis if we increase awareness, speed up diagnosis, and provide families with more support. Despite the length of the road, we are getting closer to a world free from the weight of tuberculosis with every step.
References
- National Guidelines for Management of Tuberculosis in Children
- MDPI. “Cancers | Full-Text | Analysis of Gene Expression Data.” MDPI Cancers, 12, no. 9, 2024. https://www.mdpi.com/2079-9721/12/9/202.
Read more…
How to Accurately Determine Iodine Content in Edible Salt: A Comprehensive Guide | Titrations.


